Fear of pain is the number one reason people put off dental treatment. And tooth extractions tend to sit at the top of that fear list. The word alone is enough to make some patients cancel appointments they genuinely need. But here’s the honest truth: the procedure itself is almost always far more manageable than people expect. What hurts more, in most cases, is the tooth that needed to come out in the first place.
Modern dentistry has significantly changed the extraction experience. Local anesthesia is highly effective, sedation options exist for patients with more pronounced anxiety, and aftercare has become more precise. Knowing what actually happens before, during, and after takes a lot of the fear out of the equation.
This guide walks you through the full picture: what to expect during the procedure, how pain is managed at every stage, and what recovery genuinely looks like for most patients.
What Actually Happens During a Tooth Extraction
For patients considering a tooth extraction in Midwest City, the most common concern is simple: Will I feel it? The short answer is no, not the removal itself. Here’s why.
Before anything begins, the area is numbed with a local anesthetic (like lidocaine or a similar agent) delivered via injection near the tooth and surrounding nerve. The injection itself can cause a brief sting, which dentists often minimize by applying a topical numbing gel to the gum first. Once the anesthetic takes effect, which usually happens within a few minutes, the tooth and surrounding tissue are fully numb.
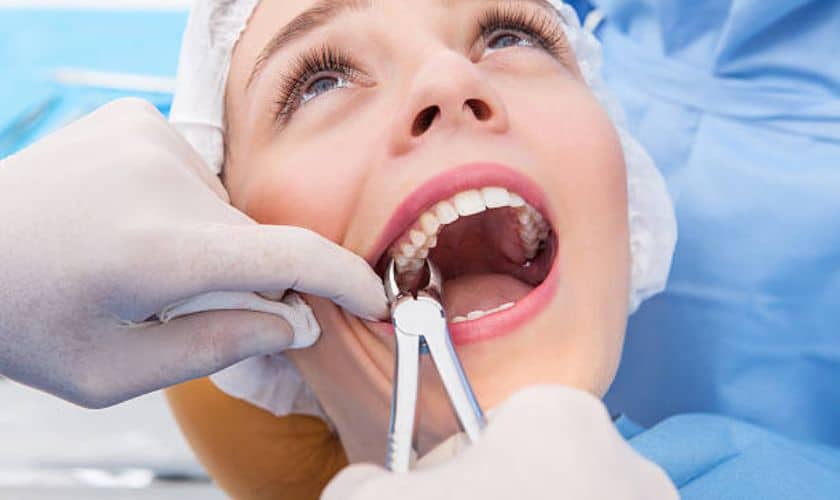
During the extraction, you’ll feel pressure and movement as the dentist widens the socket and loosens the tooth, but no pain. That distinction matters. Many patients are surprised by how much physical sensation occurs without any actual discomfort. The tooth is made free from the socket with instruments called elevators, then removed with forceps. For simple extractions, this process takes only a few minutes.
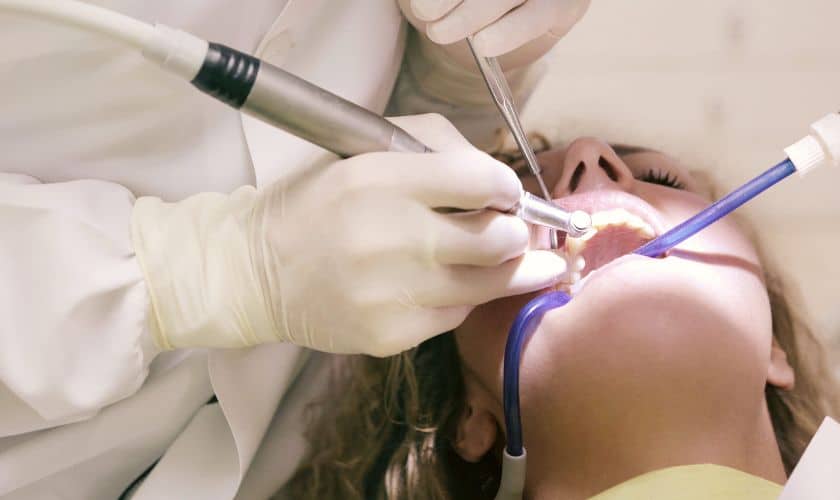
Surgical extraction is required when a tooth is impacted, broken at the gumline, or has curved roots. A small incision is made in the gum tissue to allow access to the tooth, and the tooth may be sectioned into pieces for easier removal. The procedure takes longer, but the same anesthetic principles apply. You’ll be thoroughly numb throughout.
Pain Management Options: What Midwest Smiles Offers
Local Anesthesia: The Foundation of a Pain-Free Procedure
Local anesthesia is the standard of care for virtually all dental extractions. It’s predictable, fast-acting, and highly effective. The anesthetic blocks nerve signals in the targeted area, so pain signals can’t reach the brain. For most patients, this alone is sufficient to make the procedure comfortable.
If you feel any discomfort during the procedure after the anesthetic has been applied, it’s important to say so immediately. Your dentist can administer an additional numbing agent. There’s no need to tough it out — ensuring you’re properly numb serves everyone, including your dentist, who can work more efficiently when a patient is relaxed and comfortable.
Sedation Dentistry: When Anxiety Needs More Than Numbing
For patients with significant dental anxiety, local anesthesia addresses the physical pain but not the psychological experience of being in the chair. Sedation options can help with that. Nitrous oxide — commonly called laughing gas — is a mild inhalation sedative that produces a relaxed, mildly euphoric state while keeping you conscious and responsive. It wears off quickly, typically within minutes of the mask being removed, allowing most patients to drive home afterward.
Oral sedation — a prescribed medication taken before the appointment — produces a deeper state of relaxation. Patients remain conscious but feel drowsy and often have limited memory of the procedure afterward. This option requires someone to drive you home and is typically reserved for more complex procedures or significant anxiety. Ask about the sedation options available for your specific appointment.

What Recovery Actually Looks Like And How to Make It Easier
The procedure itself is the easy part for most patients. Recovery during the hours and days after is when discomfort is more likely to appear. Understanding the typical timeline makes it much less alarming.
The First 24 Hours: What to Expect and What to Protect
Once the anesthetic wears off (usually within two to four hours after the procedure), you may notice soreness, tenderness, and swelling around the extraction site. This is a normal inflammatory response, not a sign that something went wrong. For most simple extractions, over-the-counter anti-inflammatories like ibuprofen are effective. Your dentist may also prescribe a stronger pain reliever for surgical extractions.
The first 24 hours are also the most critical for clot formation. A blood clot forming in the socket marks the beginning of healing – it protects the bone and nerve endings beneath. Protecting that clot means:
- Biting gently but firmly on gauze for 30 to 45 minutes after leaving the office
- Avoiding rinsing, spitting forcefully, or using a straw – all of which can dislodge the clot
- Keeping your head slightly elevated when resting to reduce swelling
- Applying an ice pack to the cheek in 20-minute intervals during the first day
- Eating soft foods only, like yogurt, mashed potatoes, scrambled eggs, and soup

Days Two Through Five: When Most People Turn the Corner
Swelling typically peaks around 48 hours and then begins to subside. By day three or four, most patients report significant improvement. Soreness fades, swelling decreases, and the diet can gradually expand. Gentle warm saltwater rinses (starting 24 hours after the extraction) help keep the socket clean and promote healing.
Most patients return to their normal routine within a few days, with full soft-tissue healing typically occurring within 1 to 2 weeks. Bone healing at the socket continues more gradually, over several months.
Dry Socket: The Complication Worth Knowing About
Dry socket (called alveolar osteitis) is caused when the blood clot that is formed in the extraction socket is dislodged or is dissolved before healing is completed, and the underlying bone and nerves are left exposed. It affects roughly 2% to 5% of all extractions, according to the American Dental Association, and a higher percentage of lower wisdom tooth removals.
The common sign is a sharp, throbbing pain that begins 2 to 4 days after the procedure. The pain worsens rather than improving, often radiating to the ear or jaw. If that describes what you’re experiencing, call your dental office right away. Dry socket is treatable: the dentist will clean the socket, place a medicated dressing that provides near-immediate pain relief, and guide you through the remaining healing process.
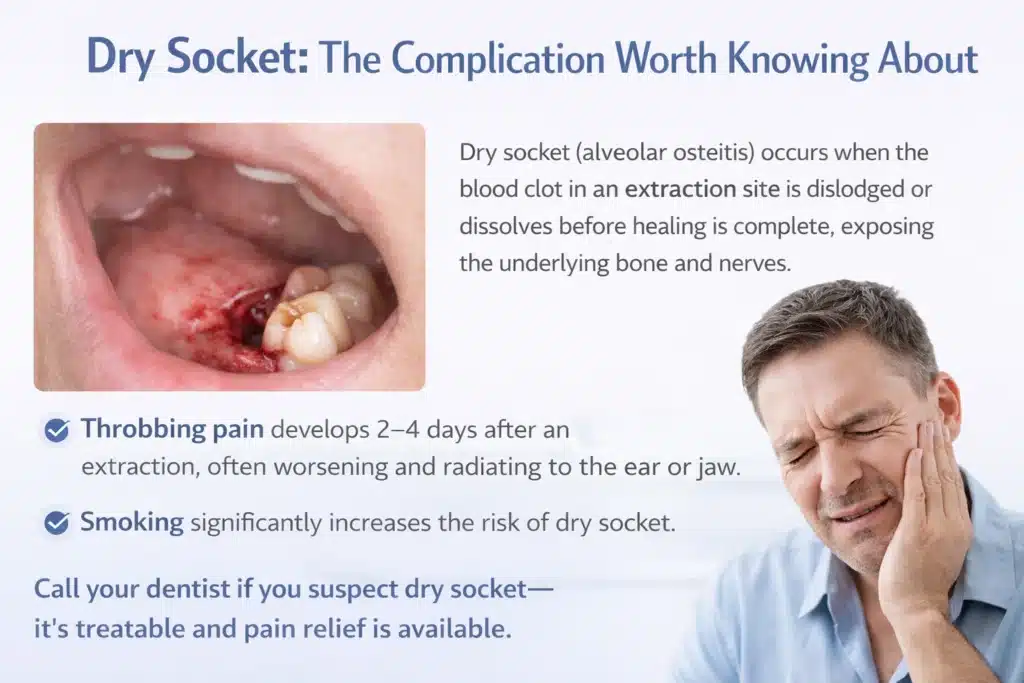
Smoking significantly increases dry socket risk; it’s one of the most important reasons dentists advise against smoking for at least 48 to 72 hours after an extraction. For residents in Midwest City managing extraction recovery while navigating a busy daily schedule, this is worth taking seriously.
Don’t Let Fear Delay Treatment You Need
Dental anxiety is real, and it’s understandable. But avoiding an extraction your mouth genuinely needs tends to make things harder – not easier. Infections spread. Pain worsens. Options narrow. Getting it handled sooner usually means a simpler procedure and a faster recovery.
Midwest Smiles provides tooth extraction in Midwest City with a team that takes patient comfort seriously – from the initial numbing to post-procedure follow-up care. Call us today or book your appointment online at midwestsmilesok.com. Whatever’s been keeping you from the chair, we’re here to help you through it.
People Also Ask
A simple extraction of a fully erupted tooth often takes less than 30 minutes from start to finish, including numbing time. Surgical extractions for impacted teeth, complex root structures, or teeth requiring sectioning can take 45 minutes to an hour or more, depending on the complexity. Your dentist will give you a realistic time estimate at your consultation.
For simple extractions without sedation, many patients return to desk work the same afternoon. If you had sedation, you’ll need the rest of the day to let the medication clear your system, and you cannot drive. Physical labor or any activity that significantly raises your heart rate is best avoided for at least 24 hours, as elevated blood pressure can disrupt clot formation. A light day is the safest approach regardless.
Soft foods are recommended for the first several days. Most patients can reintroduce firmer foods — avoiding the extraction side — by day four or five, once swelling has reduced, and tenderness is manageable. Hard, crunchy, or sharp-edged foods should be avoided until healing is more complete, typically 1 to 2 weeks. Your dentist will give specific guidance based on your individual case.
Multiple extractions in a single appointment are sometimes recommended to minimize the total number of visits and anesthetic exposures. Recovery might be a bit more time-consuming with swelling, diet restriction, and a longer healing timeline. Your dentist will weigh whether a single appointment or staged extractions makes more sense based on the number of teeth, their positions, and your overall health.
Some oozing and blood-tinged saliva is normal for the first several hours. Ongoing bleeding necessitates attention. Bite down firmly on clean gauze for 30 minutes. If that doesn’t control it, try biting on a moistened tea bag; tannic acid in black tea can help promote clotting. If significant bleeding continues beyond that, call your dental office or visit an urgent care facility. Don’t wait it out if something feels wrong.